Telemedicine, the ability to remotely treat patients in far-flung corners of the world, was still in its infancy in 1998 when it was put to a highly publicized test aboard a storm-tossed sailboat in the Southern Ocean.
Russian competitive sailor Viktor Yazykov was participating in the solo Around Alone Race. His boat was about 900 miles below the tip of South Africa when his rig began falling apart. While Yazykov was repairing a broken shroud, an elbow he had injured earlier in the race grew inflamed with infection.
Yazykov knew he needed to take quick action. He contacted race officials, who relayed his message to Dr. Daniel Carlin, a former U.S. Navy physician who two years earlier had founded Voyager Medicine to remotely treat ships crews.
Carlin emailed Yazykov specific instructions via Inmarsat C satellite, but delays in this form of communication nearly cost Yazykov his life. On the brink of collapse, Yazykov followed Carlins instructions. He lanced the pus-filled abscesses on his arm, and then treated the bleeding. A new approach to offshore medicine was born.
Sixteen years later, telemedicine is an essential part of offshore racing. Its also quicker. In the 2010 Velux 5 Oceans race, a similar service, Medical Support Offshore, based in the United Kingdom, offered assistance to Polish sailor Zbigniew Gutek Gutkowski after he sliced his head on his wind generator. Thankfully, prior to the race, doctors from Medical Support had trained Gutkowski how to handle just such an emergency.

Today, Carlin operates WorldClinic, a company based in New London, N.H., that provides clients around the globe with emergency telemedicine services. Telemedicine is not just for emergencies in faraway countries. Domestic demand for remote monitoring services is prompting a range of new technologies, many of which can benefit cruising sailors.
The establishment of clinics in rural regions that lack doctors and hospitals has become a driving force in the growth of telemedicine. The field is often referred to as tele-health or e-health when applied to non-emergency purposes.
Telemedicine is more than just an ability to call a doctor for advice. New technology has made it possible for medical professionals to use sophisticated instruments to monitor the health of their patients from a distance, in many cases, hundreds of miles. Tele-health services serve sparsely settled regions of the Midwest, northern Maine, New Hampshire, Vermont, and other states bordering Canada, as well as in prisons and areas populated by migrant farm workers.
Remote sensing devices, often located in a patients home, can record blood pressure, heart rate, glucose levels, and other health indicators, while Web cameras linked to high-speed networks provide a real-time view. This tele-presence works best when a high-speed fiber-optic cable carries the video and data signals, but increasingly, these devices are being employed at sea via satellite, with some limitations.
What does this mean for cruising sailors? Many cruisers are older, more vulnerable to injury or tropical illness that might be a mere nuisance to a younger sailor. Some suffer chronic illnesses-such as diabetes, high blood pressure, or Parkinsons disease-that require monitoring. In a nutshell, telemedicine offers cruisers a safety net that didn’t exist a few decades ago.
Uplinks and Downloads
The range of diagnostic equipment available to sailors is still slim, and the cost of this equipment is very high, but that is changing.
Any boat that wants to fully avail itself of a remote medical service will need enough power to run a laptop computer and Satcom system. According to Dan Richards, founder and chief executive officer of the Boston-based crisis management firm Global Rescue, onboard systems can range from a laptop computer costing a few thousand dollars, to one hooked to smart laryngoscopes and stethoscopes, which add thousands to the total cost.
It all depends on what you want to spend and what you want to lug with you, Richards said. Video, he explained, is not essential. We handle a number of telemedicine cases using fixed images [sent by the patient].
More expensive systems can quickly send fixed images back and forth, allowing doctors to view the patient almost instantaneously in high resolution. This gives doctors or paramedics key information they might not have without an image. Video images can provide information as well, but quality depends on bandwidth-the transmission speed measured in bits per second. Resolution on these sea-borne videos tends to be soft or grainy, and the images sent via streaming video lag behind real time.
Government researchers, including those working with the International Space Station and its undersea counterpart, Aquarius, are working to resolve latency issues, because any form of tele-surgery (surgery conducted remotely) would require live, high-speed video.
When Global Rescue needs a medical diagnosis in a hurry, it relies on a partnership with John Hopkins Hospital in Baltimore, Md., where doctors are on standby via Satcom. The hospital has a Division of Special Operations that gives Global Rescue access to the same type of services used by the U.S. Marshal Service or the U.S. Secret Service.

The satellite phones we have tested have global reach (PS, January 2012), but they still can’t transmit large amounts of data, an obstacle for live (streaming) video. New software technology is helping to overcome those limitations, but until the bandwidth issue is solved, telemedical services will rely mostly on text and voice communication coupled with still images.
Patrick Deroose, general manager of International SOSs Corporate Assistance Division, said existing satellite connections typically transmit a series of sequential still photos, as opposed to video. While the images help, he said, voice communication with a doctor is invaluable. Talk first, then discuss the photos, he said.
Although ships can be diverted to help, Deroose said many sailors have unrealistic expectations regarding at-sea evacuations. You can’t expect the Hollywood version of a helicopter coming out of the blue sky to rescue you, he said.
International SOS gets calls from ships and sailors every day. While some companies route calls to nurses or paramedics, SOS works exclusively with medical doctors. Several of its clients are commercial shipping companies who recognize that a remote diagnosis and treatment saves money, because the ship doesn’t have to make a costly diversion to a port for medical treatment.
The success of any remote medical service hinges greatly on the preparations made before a boat leaves port. One or more crew should have basic first-aid training, and the boats medical kit should be stocked with medicines and supplies that might be needed.
Tom Milne, relationship manager for corporate logistics and executive services at Seattle-based Remote Medical International (RMI), described how the companys database allows them to quickly identify who is calling for help and what medical supplies are on board. These records help the remote doctors to quickly select treatments available to the crew.
If the call indicates a severe medical problem, the RMI communications center confers with emergency room doctors and specialists at George Washington University.
Remote Diagnostic Devices
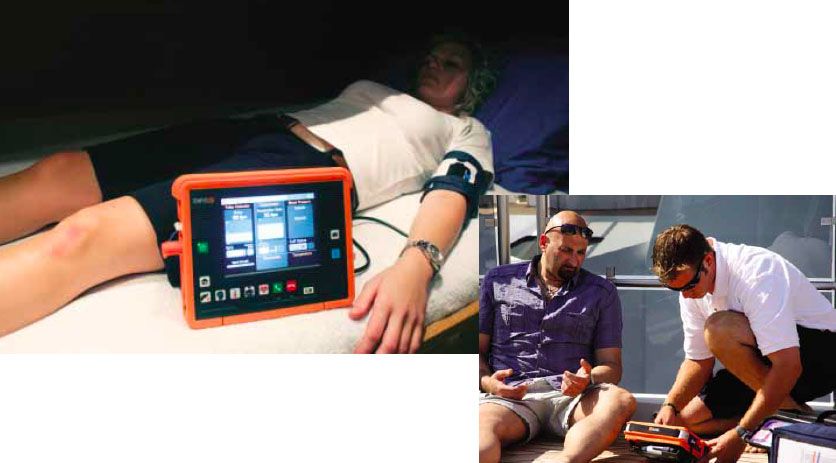
A variety of portable systems have been developed to transmit data from remote medical diagnostic devices. For the past 10 years, RDT, manufacturer of Tempus medical equipment, has been developing monitors capable of sending data from at sea or in the air to doctors on land.
Yacht captains and airline pilots can now hook up a crewmember or passenger to a portable Tempus monitoring device, which collects data that would otherwise be gathered by emergency room personnel-blood pressure, ECG, pulse and respiration-and quickly transmit it. This allows doctors to better manage the incident and decide what steps to take. Without such a device, time is often wasted while those at the scene attempt to simultaneously monitor and relay the patients vital signs to doctors.
The newest Tempus devices have been designed to integrate with onboard communications equipment. The system is already in place on some airlines.
In 2003, 50-year-old passenger Stephen Clarke developed chest pains while flying from Chicago to Manchester, England. The cabin staff used a Tempus device to record his vital signs and beamed the data by satellite to ground-based doctors in Arizona. The physicians diagnosed a heart attack and instructed flight attendants how to give emergency treatment. Clarke became the first commercial air passenger to have a live echocardiogram (ECG) recorded in-flight.
DigiGone, another firm offering medical monitoring devices for use in the field, combines a remote viewing station and encrypted communications software with portable diagnostic equipment to directly link to the patients telemedicine service provider.
When it comes to compact, medical sensing devices built for rugged service, California-based Human Edge Technology is at the cutting edge. Its lightweight, user-friendly software and hardware solutions provide sensing and Satcom service in the most extreme environments. Human Edge has tested its gear first-hand on expeditions to the Himalayas, in the Amazon, Antarctica, and on ocean crossings.
The company offers an expedition communication package that includes a laptop, satellite phone with cables, and collapsible solar panels, all tucked into a Pelican case. Its Polar High-speed Data Package is designed to provide live video conferencing. The box weighs 25 pounds and costs about $6,000.
Human Edge founder Tom Sjogren said its the only device of its kind operating in polar regions outside the Inmarsat satellite system footprint.
The Future
While this equipment is well beyond the reach of ordinary sailors today, a future in which we can get a full checkup using a doctor ashore while underway isn’t as far away as it seems. For a glimpse of this future, we need look no further than the U.S. military. The Telemedicine & Advanced Technology Research Center (TATRC), an office of the U.S. Army Medical Research and Material Command, is exploring the many ways telemedicine can support its soldiers. Its projects include a highly mobile humanoid robot known as the BEAR robot, which is designed to rescue fallen soldiers on the battlefield.
The research center also examines the technology that can enable a surgeon to remotely perform an operation using a computer-operated robot. One active example of these surgical robots is called DaVinci, made by Intuitive Surgical in Sunnyvale, Calif. Already in use at Walter Reed Army Hospital in Washington, D.C., DaVinci has limbs that can be guided by a surgeon who sits at a console in the same room. The surgeon views the operation via three-dimensional imagery supplied by the robots cameras.
Although such relatively large and expensive robots may seem of little value aboard a cruising sailboat today, miniaturization and lower costs are opening up new possibilities for what may one day be standard equipment.
Currently, the biggest challenges to tele-robotic surgery are linked to limited bandwidth, which slows down data transmission speeds. There is simply too much lag time via satellite between the field medic (or robot) and doctors at the hospital or command center on the far side of the world. While these connectivity problems are surmountable, one fixed limitation-the speed of light-will remain a problem for procedures performed by surgeons thousands of miles away.
For several years, Human Edge has been searching for inexpensive ways to boost bandwidth. By linking two Inmarsat 9202 satellite phones together, using a Hughes BGAN router and a second router in the Cloud, they have achieved respectable data transmission speeds of up to 800 kilobytes per second. By connecting three of these Satphones, the speeds exceeded 1 megabyte, or (1,000 kilobytes), the minimum for video transmission.
This modular approach helps bring down the cost, but its still not cheap. The Human Edge system with Satphones, laptop, solar panel, batteries, and a few accessories sells for less than $4,000, and this doesn’t include the data transmission plan, which can add up quickly, depending on usage. Weight, which varies depending on equipment, is about 18 pounds, but that is coming down.
The trend is moving toward iPhones and Androids and getting away from heavy, power-hungry units like [ruggedized laptops], Human Edge founder Sjogren said.
While telemedicine providers are optimistic about the future, they agree that sailors will still have the biggest responsibility for their own health. Without pre-training and a good onboard medical kit, even the best advice will be of limited help.

In the final installment in our fourpart series on seagoing medical kits in 2008, we evaluated pre-packaged offshore medical kits for boats undertaking ocean passages. A few of the kits we looked at were meant to be combined with telemedical services. Here are some highlights from that article (PS, December 2008), which examines exactly what sailors should have on board.
- Our Best Choice for offshore sailors, the Adventure Medical Marine 3000, contains seven injury- or sicknessspecific modules, including dental, wound care, medicine, bleeding, CPR/ instrument, blister/burn, and fracture/ sprain. Each module is clearly identified with its contents easily viewed via a large vinyl window.
- Ocean Medical International’s Class A kit includes a grab bag for initial responses to medical emergencies. It was the most comprehensive kit in our test and the only one that came with a defibrillator. OMI also offered a 24/7 medical support via phone or email.
- The list of supplies in the Trans-Ocean Pak from Fieldtex is extensive. It contains 13 separate modules, each one dedicated to a particular kind of injury or illness.


































